Neurac® Therapy
Restore movement. Relieve pain. Enhance performance.
Neurac Therapy is a research-supported approach to rehabilitation and everyday life performance training. It targets the root causes of pain and dysfunction by aiming at restoring proper neuromuscular control — through precise suspension exercises with vibration and gradual pain-free progressions.
The "Neurac" name is short for neuromuscular activation, and coins that the approach specifically targets the nervous system's control of the motor system.
Neurac Therapy is the clinical application of the Neurac® Method for patients with neuromusculoskeletal pain, dysfunction, or performance limitations. It uses standardized suspension-based exercise tests to assess and treat, while re-testing performance in a relevant functional task to support or challenge the clinical hypotheses.
Neurac Therapy is delivered by licensed healthcare practitioners—such as physical therapists, chiropractors, physicians, and equivalent regulated professions—who have completed Redcord’s structured Neurac education program consisting of three progressive courses taught by certified instructors.
Within Neurac Therapy, clinical hypotheses are explored directly during task performance by temporarily influencing how the task is performed. This approach is called Perform Pluss (Perform+).
Perform+ refers to a therapist-led strategy in which task conditions are intentionally modified in order to observe immediate improvement in movement quality and symptoms. The goal is to test, support, or weaken a working clinical hypothesis.
Perform+ refers to changes that temporarily support or facilitate task performance.
The therapist may guide Perform+ through manual contact, verbal instruction, or changes to the body–environment interaction, such as external support, altered stance, or modified load. Most often specific kinetic chain activation is manipulted and immediate changes in functional task performance inform further assessment and treatment decisions.
A functional task is a movement activity that replicates what the patient reports having difficulty performing in daily activities or sport-specific contexts and is therefore meaningful to the patient (Zarzycki et al., 2022). Examples include reaching onto a shelf, putting on a shoe while standing, lifting an object, walking, running, or changing direction.
During functional tasks, movement quality reflects how effectively the body’s stability and mobility systems interact to meet task demands. According to the combined stability–mobility systems model, effective movement depends on coordinated interaction between stabilizing and mobilizing subsystems, and changes in task conditions can immediately alter this interaction (Hoffman et al., 2013).
The therapist deliberately manipulates task conditions—through manual contact, verbal instruction, or changes to the body–environment interaction—to test clinical hypotheses.
Manual contact, verbal instruction, or external items may be used to alter task performance, with immediate changes guiding further assessment and treatment.
A functional task is a movement activity that replicates what the patient reports having difficulty performing in their daily activities or sport-specific context, and is therefore meaningful to the patient (Zarzycki et al., 2022).
For example: reaching on a shelf, putting on a shoe while standing, lifting a frying pan, walking, running, or cutting.
In functional tasks, movement quality reflects how effectively the stability and mobility systems interact to meet task demands (Hoffman et al., 2013).
-
Perform+ temporarily improves that interaction.
According to the combined stability and mobility systems model, movement quality depends on effective interaction between stabilizing and mobilizing subsystems, and altered task conditions can immediately change this interaction (Hoffman et al., 2013).
How Perform+ is used in Neurac Therapy
1. Select a functional task
Choose a specific task the patient reports difficulty performing in daily life or sport (e.g. bending down to pick up an object).
2. Observe baseline performance (CASSS)
Assess Control, Amount of movement, Speed, Symmetry, and Symptoms during the task to establish a reference.
3. Apply Perform+ (facilitation)
Temporarily facilitate the task by adjusting task conditions—through manual contact, verbal instruction, or changes to the body–environment interaction—and repeat the same task.
4. Choose Neurac tests, treat, and re-test the task
Use the observed CASSS responses to select relevant suspension-based test/exercise(s) (e.g. Supine Pelvic Lift, Prone Bridge). After treatment, re-test the original functional task to support or challenge the clinical hypothesis.
Immediate changes in task performance help guide exercise selection and progression within Neurac Therapy.
Clinical example
A patient reports pain when bending down to pick up a paper. The clinician observes reduced control (e.g., jerky movement or deviant load transfer), limited range of motion, and pain during the task.
With Perform+, the clinician temporarily improves trunk–pelvis support (e.g., manual abdominal pressure, a simple cue, or an external constraint) and repeats the same task. If pain decreases, control improves (e.g., improved force-steadyness), and the patient reaches further with less hesitation, this supports the hypothesis that task performance is sensitive to trunk–pelvis strategy.
The the findings guide the next step in Neurac Therapy—often progressing into standardized suspension-based tests such as Supine Pelvic Lift and Prone Bridge, followed by immediate re-testing of the functional task
The clinical example elaborated
The abstracted example above are elaborated into a more practical or concrete one, including:
-
The functional task
-
The hypothesis
-
Perform+ variants (manual, verbal, environmental)
-
Perform– variants (safe challenge)
-
Exactly what outcomes to look for (CASSS + simple measures)
-
And how this translates into Neurac testing (Supine Pelvic Lift / Prone Bridge)
Example: Using Perform+ during a functional task
Functional task
Standing forward bend to pick up a paper from the floor.
This task is selected because it replicates a daily activity the patient reports difficulty performing (cf., "History").
Step 1: Observe baseline task performance
The patient performs the task two to three times. The therapist observes baseline performance using the CASSS factors (Control, Amount, Speed, Symmetry, Symptoms) [Zarzycki et al., 2022]:
-
Control: movement smoothness, coordination, guarding, segmental “buckling”, or abnormal pelvis-hip or scapulo-humeral rythm.
-
Amount: how far the patient can bend (for example fingertip-to-floor distance in centimeters)
-
Speed: ease and continuity of movement, hesitation, stop–start behavior, or number of seconds to perform the task.
-
Symmetry: weight shift, hip shift, trunk rotation, or one-sided avoidance (pick with right and left hand).
-
Symptoms: pain (rated on a 0–10 Numeric Rating Scale), fear (dreadful face), or discomfort (moaning, stating)
Simple outcome measures (sufficient for clinical decision-making) [cf. CASSS]:
-
Brief movement control description (smooth / hesitant / segmented) [C]
-
Fingertip-to-floor distance or reach distance (A)
-
Seconds taken to perform the task (S)
-
Presence or absence of side-to-side asymmetry (S)
-
Pain score (0–10) [S]
Step 2: Form a working hypothesis
Rather than attributing findings to isolated muscle “activation,” the hypothesis is framed in terms of movement strategy and load transfer:
Hypothesis:
The patient’s symptoms and movement quality during the floor pick-up are influenced by insufficient control and force transfer between the trunk and pelvis under load. If trunk–pelvis support is temporarily improved applying fascilitation measures, task performance should improve immediately, as reflected by changes in Control, Amount, Speed, Symmetry, and Symptoms. Reverse effects should be registered appling inhibation measures.
Step 3: Apply Perform+ (facilitation)
Perform+ (A): Manual abdominal support
The therapist provides gentle, broad support at the lower abdomen or pelvis (similar to a light brace), and the patient repeats the task.
What this tests:
Whether temporarily improving trunk–pelvis support improves task performance.
A positive Perform+ response may include:
-
Reduced pain (for example a decrease of two points or more on the pain scale)
-
Smoother descent and return, with less guarding
-
Increased reach toward the floor
-
Less hesitation during the movement
-
Reduced trunk rotation or side shift
Perform+ (B): Instructional facilitation (no manual contact)
The therapist provides simple verbal instructions, such as:
-
“Breathe out gently as you start to bend.”
-
“Keep your rib cage stacked over your pelvis.”
-
“Lightly brace as if preparing for a cough, without holding your breath.”
The task is then repeated.
Purpose:
To test whether a cue-led change in movement strategy improves task performance.
Perform+ (C): Change in body–environment interaction
A temporary belt, strap, or light tactile band is applied around the lower trunk or pelvis, and the task is repeated.
Purpose:
To test whether altering external task conditions improves performance without therapist contact.
Step 4: Translate findings into Neurac testing and treatment
If Perform+ targeting the trunk–pelvis region is clearly positive, and facilitation targeting the hips or feet is negative, the next logical step in Neurac Therapy is to select suspension-based tests and exercises that challenge trunk–pelvis force transfer.
Common examples include:
-
Supine Pelvic Lift: graded testing and training of force transfer between hips, pelvis, and trunk (posterior and rotational chains dominant)
-
Prone Bridge: graded testing and training of integrated trunk stability and coordination under load (anterior and rotational chains dominant)
After treatment, the original functional task (picking up the paper) is re-tested to support or challenge the clinical hypothesis and assess carry-over.
Clinical interpretation
Improving trunk–pelvis support changed task performance immediately, suggesting that the patient’s movement strategy and load transfer during the floor pick-up are modifiable and clinically relevant. This response is consistent with, but does not directly prove, improved neuromuscular function of the trunk–pelvis-hips kinetic chains.
References
Zarzycki, R., Smith, C. A., Smith, S. S., & Van Dillen, L. R. (2022). Application of the 4-element movement system model to sports physical therapy and education. International Journal of Sports Physical Therapy, 17(1), 108–123. https://doi.org/10.26603/001c.30318
Hoffman, S. L., Gabel, P., & Williams, J. (2013). Expanding Panjabi’s stability model to express movement: A theoretical model. Manual Therapy, 18(3), 236–240. https://doi.org/10.1016/j.math.2012.10.005
Scientific studies and research
30 years of experience
Improves daily function and performance
A pain-free approach
The Neurac Method combines two main paths:
Therapy & Exercise
The Neurac Method is applied through two main professional approaches: Neurac Therapy and Neurac Exercise. While each serves a different role, they are based on the same scientific principles and equipment, and together form a complete method that supports people across all stages — from pain and dysfunction to health and peak performance.
Neurac Therapy
Neurac Therapy provides a comprehensive diagnostic and therapeutic framework designed to target neuromusculoskeletal disorders and associated pain.
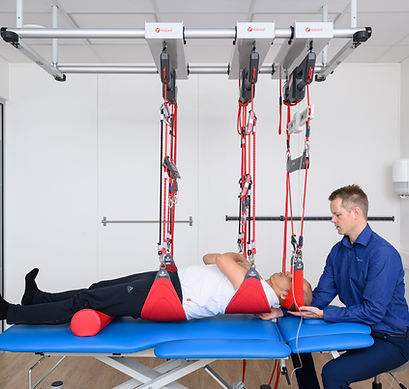
By using carefully designed sling-based exercises, the therapist activates and retrains the neuromuscular system, aiming to restore optimal motor control, improve functional movement patterns, and reduce pain.
It focuses on identifying and addressing dysfunctions in movement and muscle activation that contribute to pain or injury.
This method is primarily applied in one-to-one clinical settings, typically by healthcare professionals such as physiotherapists.
Neurac Therapy is widely used in rehabilitation, both for acute injuries and long-term conditions, and forms the clinical foundation of the method.
Documented Benefits of Neurac Therapy
-
Neurac Therapy is level 1 evidence based [1] for the effect on low back pain [2-6] and stroke rehabilitation [7]
-
Neurac Therapy is ranked among the top therapies for pain relief for low back pain [2-4].
-
Neurac Therapy is significantly more effective than all comparisons for muscle strength, activation, and onset for low back pain [5].
-
Neurac Therapy is superior to passive treatment and other exercises both short- and long-term for low back pain [6].
-
Neurac Therapy is more effective on walking ability post-stroke than conventional physical therapy,and trunk training [7].
References 1. Howick, J.C., I., et al. OCEBM Levels of Evidence: The 2011 Oxford Center of Evidence-based Medicine Levels of Evidence (Introductory Document). 2011 [cited 2024 Feb 12, 2024]; Available from: https://www.cebm.ox.ac.uk/resources/levels-of-evidence/ocebm-levels-of-evidence. 2. Li, Y., et al., Exercise intervention for patients with chronic low back pain: a systematic review and network meta-analysis. Front Public Health, 2023. 11: p. 1155225. 3. Yang, J., et al., Efficacy of exercise therapy in the treatment of chronic low back pain patients: a network meta-analysis. Chin J Evid Based Med, 2021. 21(1): p. 28-39. 4. Yajing, Z., et al., Efficacy Of Exercise Combined With Conventional Therapy On CLBP Patients: A Network Meta-analysis...2021 ACSM Annual Meeting & World Congresses [Virtual], June 1-5, 2021. Medicine & Science in Sports & Exercise, 2021. 53(8S): p. 231-232. 5. Drummond, C., et al., Sling Exercise in the Management of Chronic Low Back Pain: A Systematic Review and Meta-Analysis. J Strength Cond Res, 2021. 6. Park, C., H. Jeong, and B. Kim, Effects of Sling Exercise on Pain and Disability in Patients with Chronic Low Back Pain: Meta-Analysis of Studies in Korea. J Int Acad Phys Ther Res, 2020. 11(3): p. 2155-2163. 7. Long, J., et al., Effects of sling exercise therapy o
Neurac Exercise
Neurac Exercise builds on the same core principles of neuromuscular activation, but is aimed at promoting health, performance, and injury prevention through advanced sling-based training.
While Neurac Therapy is treatment-oriented, Neurac Exercise focuses on maintaining and enhancing physical capacity — helping individuals stay healthy, build fitness, and boost performance.
Neurac Exercise provides a structured training system suitable for:
-
Prevention of injury
-
Maintenance of function and mobility
-
Performance enhancement for athletes and active individuals
It is designed for use by personal trainers, fitness instructors, and therapists who wish to integrate high-quality training into their practice. It can be applied in both individual and group settings — in gyms, studios, or clinics.

Documented Benefits of Neurac Exercise
-
Evidence-based at level 1 (systematic review) for healthy subjects and athletes [1].
-
Sling exercise activates the core muscle groups more than traditional exercises in systematic review evidence [2].
-
Closed-chain core exercise activates more groups of muscles in a kinetic chain than open-chain exercises (systematic review) [3].
-
Core exercise has:
- Very large effect on throwing/hitting distance.
-
Large effects on balance and horizontal jump.
-
Moderate effect on vertical jumping.
Compared to normal athletic activity (systematic review) [4].
-
Core exercise has a large effect on:
- Lower limb muscle power
-
Linear sprint speed
-
Change-of-direction speed/agility
-
Sport-specific performance
References 1. Howick, J.C., I., et al. OCEBM Levels of Evidence: The 2011 Oxford Center of Evidence-based Medicine Levels of Evidence (Introductory Document). 2011 [cited 2024 Feb 12, 2024]; Available from: https://www.cebm.ox.ac.uk/resources/levels-of-evidence/ocebm-levels-of-evidence. 2. Aguilera-Castells, J., et al., Muscle activation in suspension training: a systematic review. Sports Biomechanics, 2020. 19(1): p. 55-75. 3. Adeel, M., et al., Effects of Strengthening Exercises on Human Kinetic Chains Based on a Systematic Review. Journal of Functional Morphology and Kinesiology, 2024. 9(1): p. 22. 4. Rodríguez-Perea, Á., et al., Core training and performance: a systematic review with meta-analysis. Biol Sport, 2023. 40(4): p. 975-992. 5. Sæterbakken, A.H., et al., The Effects of Trunk Muscle Training on Physical Fitness and Sport-Specific Performance in Young and Adult Athletes: A Systematic Review and Meta-Analysis. Sports Med, 2022. 52(7): p. 1599-1622.
How Therapy and Exercise Work Together
Both Neurac Therapy and Neurac Exercise are grounded in the same scientific principles and use the same high-quality equipment, ensuring a consistent and effective approach across the entire continuum of care.
Together they complete the method by supporting a continuum of care: from careful rehabilitation to tough long-term health and peak-performance exercise.

Developed through clinical practice
Our therapists work constantly to further develop the NEURAC treatment method at our competence center, Redcord Clinic in Oslo. Redcord Clinic is the key element in the development of our concept and putting our treatment method into practice through individual rehabilitation, training, and consistent follow-up with patients
Curious about Redcord?
Interested in learning more about our equipment or exploring our courses?
Whether you have questions about our innovative therapy and exercise solutions or want to discover how Redcord can help you reach your goals for patient outcomes, our team is ready to help.
Please provide information about your market, specific requirements, and any relevant details so we can serve you better.